This is a MedPage Today story.
In the wake of the Supreme Court’s ruling on Roe v. Wade, doctors across the country are facing an array of legal questions and concerns that are so new and uncertain they once seemed out of the realm of possibility, according to experts.
From determining whether they can provide care when the life of the mother is at risk and whether they must report a patient for a self-induced abortion, to considering how to code certain medical treatments and how to avoid allegations of aiding and abetting, doctors – – and other healthcare providers and staff — are finding themselves caught in a precarious legal framework that is still in flux.
“It is a horrible situation to put doctors in, who really just want to help patients,” Jessie Hill, of Case Western Reserve University School of Law in Cleveland, Ohio, told MedPage Today. “But at the same time, they have to abide by the law.”
The state-by-state complexities of trigger bans that went into effect once Roe was overturned have made matters exceedingly difficult for doctors, Hill and other experts said. Some trigger bans are being challenged, putting several states in legal limbo, while new laws that ban abortions in other states could pop up. Additionally, state legislatures could move immediately or in the coming months to make anti-abortion laws even stricter, threatening access to contraception and in vitro fertilization.
All the while, the laws have been and continue to be written by politicians, not physicians, experts noted. And because enactment and enforcement of the laws are unprecedented, there isn’t an existing branch of law dedicated to helping doctors and other healthcare professionals navigate them.
What is certain, however, is that the stakes are incredibly high for physicians, who can face losing their licenses, as well as felony charges and substantial prison time for a variety of newly minted, rapidly changing, and often vague laws.
“Healthcare has so many rules and so many regulations,” Hill said. “But most healthcare rules and regulations don’t carry criminal penalties.”
From state to state, potential penalties can be levied for anything from directly providing an abortion, to simply providing a phone number to a woman seeking medical care. As physicians grapple with this new scrutiny, experts are certain their patients will suffer greatly as well.
“I think it’s really going to chill the provision of care,” Hill noted.
Navigating patient care, and so much more
Experts detailed a handful of areas that doctors will need to seek legal guidance or counsel for in the days and months ahead. There will no doubt be more to come, as well as many intricacies under each category.
“This is such a shift in the law and the framework that we’ve all been grounded in for such a long time,” Katie Keith, of Georgetown University Law Center in Washington, DC, told MedPage Today. “People could always practice medicine in the way that they needed to.”
Now, doctors are going to be looking over their shoulders and second-guessing what they’re doing, she said.
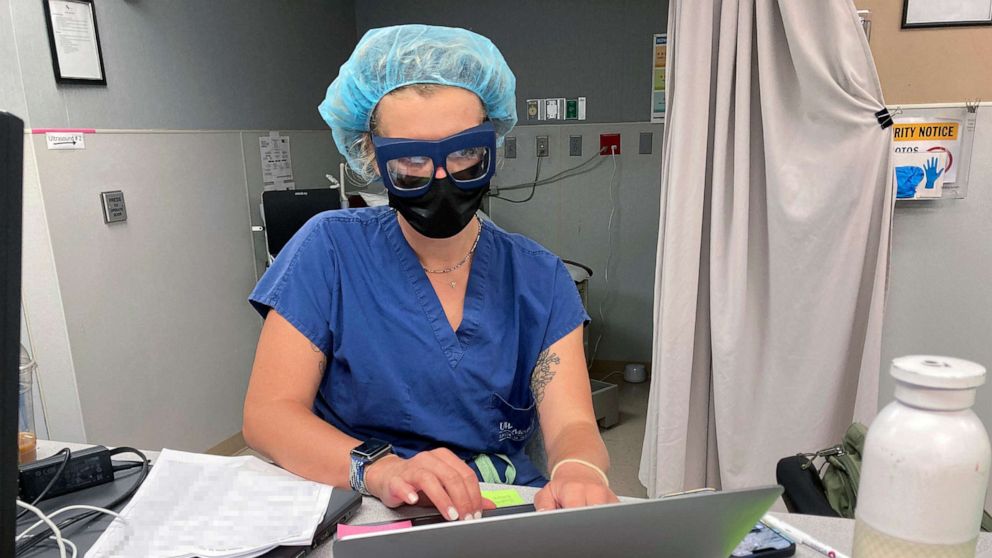
A doctor updates files between performing abortions at the Trust Women clinic in Wichita, Kan., on June 24, 2022.
Roxana Hegeman/AP
One critical question involves saving the life of the mother — how is that being defined, and how broadly or narrowly can physicians interpret it in states that ban abortions but allow for such an exception?
“How ill does someone have to be?” Keith questioned. Conditions can range from preeclampsia to ectopic pregnancies.
One potential loophole may be the Emergency Medical Treatment and Labor Act (EMTALA), a federal law enacted in 1986, Keith noted. EMTALA requires emergency departments that receive Medicare or Medicaid funding to stabilize patients.
At the same time, due to uncertainties surrounding the new laws, doctors may have to question whether to help a pregnant woman who is losing massive amounts of blood, and whether to treat a woman who has been diagnosed with cancer and needs to terminate her pregnancy in order to start chemotherapy, she explained.
“My concern is that doctors will feel constrained, and that it will have a chilling effect and that women who should qualify will not be getting care,” she added.
Another area of concern is miscarriage management, experts said, such as the treatment of patients experiencing incomplete miscarriages with medication or a procedure.
Keith wondered if doctors will feel uncomfortable providing that care, pushing women to travel to another state.
Physicians and other providers will also be faced with situations in which a pregnant woman’s fetus has been found to have a fatal defect, experts noted.
“This is just so devastating,” Miranda Yaver, an assistant professor of political science at Wheaton College in Norton, Massachusetts, told MedPage Today. “Imagine a patient having to carry a fetus to term that is not going to be able to survive.”
Furthermore, healthcare providers may be elements of whether they must report patients who are experiencing abortion complications or who have attempted to induce their own abortions, Hill said.
Oftentimes, a provider may think they’re required to report something when they’re not, she added, which can become a real problem for patients.
“Is this going to hinder patients’ ability to have healthy communication with providers?” Yaver Married.
Perhaps one of the most vague aspects of some state laws is aiding and betting, experts noted.
“There’s often a very hazy line between what is First Amendment-protected counseling … and what is aiding and abetting,” said Hill.
Causes for concern could be as simple as making a referral, Keith pointed out. “We’re in uncharted waters.”
Another looming question is whether states can restrict access to or ban the FDA-approved drug for medication abortion, she added, noting that medication abortion will be an important area to watch from a legal perspective.
Keith further said that doctors will face questions regarding how reproductive care gets coded in medical records, as well as whether certain restrictions are placed on out-of-state telemedicine providers.

A sign welcoming patients from East Texas is displayed in the waiting area of the Women’s Reproductive Clinic, which provides legal medication abortion services, in Santa Teresa, NM, on June 15, 2022.
Robyn Beck/AFP via Getty Images
And if states move to include language in their laws that specify that life begins at the moment of fertilization, there could be an additional range of legal concerns for physicians and other providers, experts said.
Dr. Thomas Burwinkel, a reproductive endocrinologist in Cincinnati, Ohio, noted that he posed the following question to the legislative committee in the Ohio House: If a lab’s liquid nitrogen storage tank breaks, and all the embryos that are stored there are lost, will physicians and staff be criminally prosecuted?
“It’s a very slippery slope,” he said of proposed legislation in Ohio. “I’m having a hard enough time recruiting embryologists into the field.”
There will be many infertile patients who will not be able to get the services they need, he pointed out.
Ultimately, “abortion is the beginning, not the end,” Yaver said. “This is really foreshadowing broader concerns about contraceptive access. Some people on the right characterize Plan B and IUDs as abortive.”
Millions of patients rely on those contraceptive methods, she noted. “These gray areas are going to hurt providers, and they’re going to hurt patients.”
Seeking guidance when it really counts
Making matters all the more complicated, many doctors and clinicians may not have a ready Rolodex of legal advisors available on demand. However, answers as to what care physicians can provide are needed at a moment’s notice, and the network of new state laws is evolving just as fast.
It’s not clear that there is an obvious answer to who doctors and other healthcare providers can turn to, Hill said.
If they are employed by a relatively large institution, such as a hospital or health system, providers will look to their hospital policy or legal counsel.
“This is the twin danger of laws like this,” Hill noted. “They make doctors worry about liability, so if they can’t readily access legal advice, they are probably going to take the conservative approach. They also encourage hospital legal departments to put guidance in place to protect themselves.”
The people who have the expertise here are criminal defense lawyers, who are likely to be called upon for help before and after the fact, she said.
“We have to be honest with ourselves,” Leila Jade Levi, senior counsel for reproductive rights and health at the National Women’s Law Center in Washington, DC, told MedPage Today of the legal and medical community. “There are things we can’t know and don’t know.”
However, there are many lawyers, pro bono and otherwise, who would be available for a physician or other provider to “defend a medical decision that they have made in consultation with the patient,” she said.
Though it is not a unique problem, it is certainly exacerbated post-Roe, she noted. Physicians have long operated with medical malpractice insurance, but what the field is dealing with now is criminalization, and that landscape is changing minute by minute.
Levi said that the National Women’s Law Center and other organizations would likely take some cases on a case-by-case basis, noting that she is most concerned about the effects that the ruling and resulting state trigger laws will have on the provision of care.
Fearing the fallout and further limitations
Levi emphasized that it’s not just physicians who will be affected by the new laws — the impact will extend to nurses and administrative staff at healthcare facilities.
Think about the person who answers the phone at a clinic who has to tell the patient that it is not providing care, she said. That same person may also have to question whether they can provide a phone number to another facility for fear of legal ramifications.
Burwinkel also noted that in addition to OB-GYN and fertility providers, emergency medicine physicians will be on the front lines, as will psychiatrists and psychologists handling trauma from unwanted pregnancies and other factors.

A staff member works at the reception desk at the Hope Clinic For Women in Granite City, Ill., on June 27, 2022.
Angela Weiss/AFP via Getty Images
When it comes to how enforcement of new state laws may play out, Hill described an example of a woman’s partner or family member being unhappy about abortion-related care she received, and reporting it.
It’s also possible that healthcare professionals may be reported by their colleagues for providing certain care or services, experts said.
Overall, Hill noted that she thinks enforcement is going to be “uneven, capricious and arbitrary.”
Yaver said she believes the Supreme Court’s decision is “going to have far-reaching effects on relationships between patients and their providers and relationships between providers and states,” all to “the detriment of people’s lives.”
Where physicians select to establish their practices is going to deepen the health disparities between red states and blue states, she added.
Levi pointed out that when a patient is sick or in a precarious medical state, having to include politicians or lawyers in deciding what the best course of care is, is not only dangerous, but insulting.
It’s an “attack on both the dignity of the patient and the provider,” she said.